Malaria is a major threat to human life. Malaria has killed and debilitated humans for centuries. Though malaria rates have reduced sharply in the last 20 years, it still sickens hundreds of millions of people and is a leading cause of death around the world. But now, the first-ever vaccine against malaria is being tested in three countries where malaria is a major public health hazard. The results of this vaccine campaign and trial will have a huge impact in how the world approaches malaria prevention in the race to reach a global target of reducing malaria illness and death by 90% by 2030.
The global burden of malaria is immense. There were 219 million cases of the disease, in 87 countries in 2017. 435,000 people died of malaria that year. Malaria is especially deadly to children and pregnant women — and even when it doesn’t kill, it debilitates. The disease causes severe pain and high fever, leading to extended absence from school, the workplace or home obligations. Its economic impact is high.
In addition to being a major threat to human life, malaria is extremely difficult to control. The unique medium of malarial infection – including both a parasite and the parasite’s mosquito host – makes it nearly impossible to eliminate. At present, malaria is controlled through a whole range of different measures, including insecticide-treated bednets, indoor spraying for mosquitoes, removing the breeding grounds for mosquitoes, preventative antimalarial drugs, and identifying and treating malarial infections as fast as possible to reduce the amount of time people can spread the disease.
Researchers are approaching the problem of malaria control from all angles, considering everything from entirely eliminating mosquitoes through genetic manipulation to attempting to develop a laser that zaps mosquitoes. There is also a constant need to develop new treatments for malaria, as the parasite that causes the disease constantly evolves resistance to existing drugs. Adding a vaccine to that suite of interventions has the potential to tip this challenging balance in favor of malaria control.
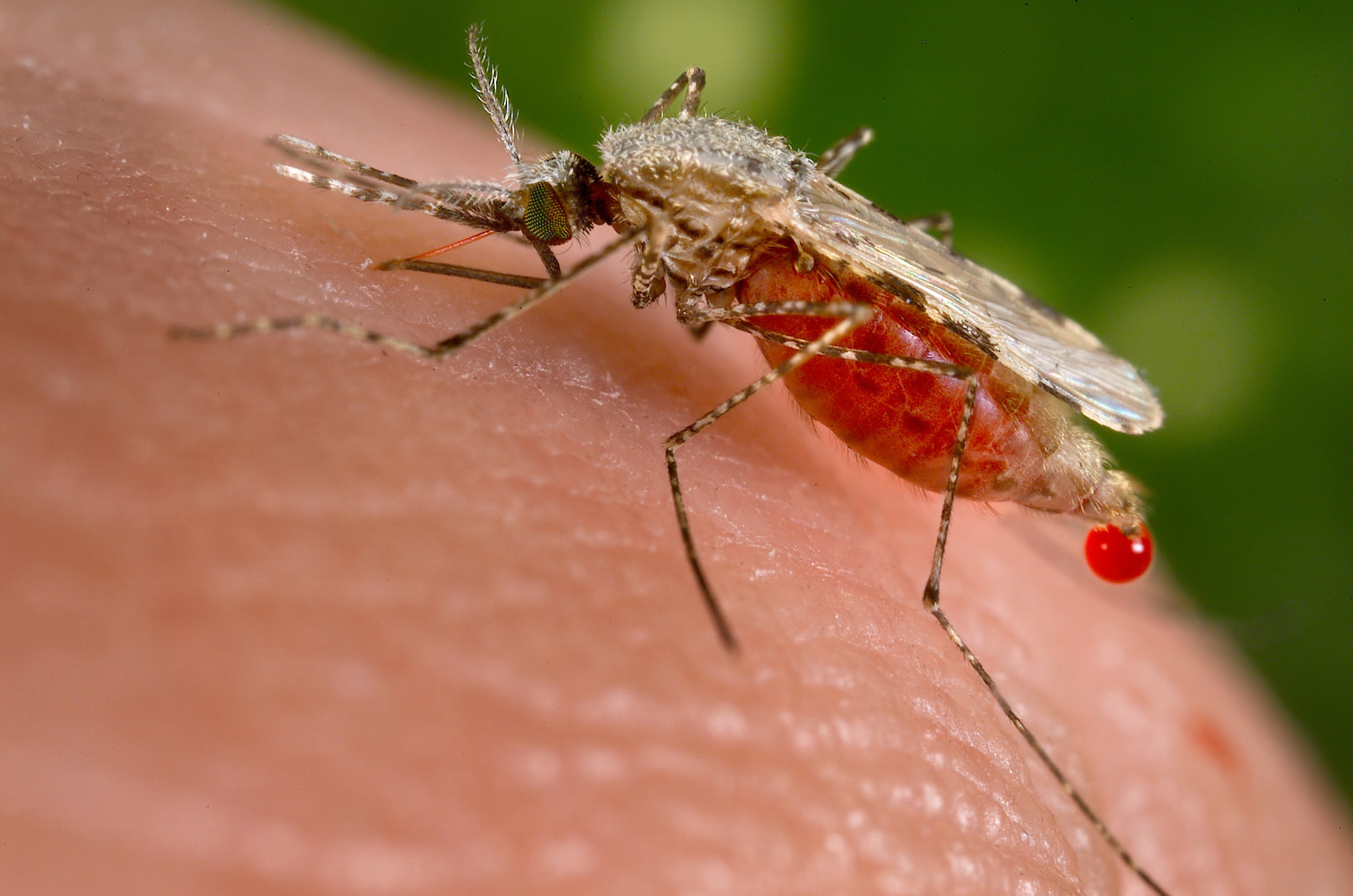
Malaria is caused by parasites called plasmodium. There are five different types of plasmodium parasites that cause malaria in humans, and P. falciparum and P. vivax are the two that cause the most infections. Plasmodium does not spread directly from person to person. Instead, it is spread through the bite of an infected Anopheles mosquito. Mosquitoes need blood to nurture their eggs; they bite humans and animals to get the blood they need. When they bite an animal infected with the plasmodium parasite, the parasites infect the mosquito. The parasites live in the mosquito, growing and multiplying. When the mosquito bites another human or animal, they pass along the infection. This lifecycle has two main implications. First, the parasite infection doesn’t seem to cause mosquitoes any great harm. They may be plasmodium hosts, but they don’t get malaria. Second, malaria has an animal reservoir. Even if you can eliminate it in the human population, they’ll always be at risk of a new zoonotic infection.
As a result, malaria control efforts focus on putting a whole set of malaria prevention interventions into place. There is no single effective anti-malaria technique – we can’t eliminate every animal that could be infected. Instead, you need a holistic set of activities – a toolbox with a whole collection of different tools to deploy as needed. Programs that substantially reduce the spread of malaria, such as Brazil’s Project for Control of Malaria in the Amazon Basin (PCMAM) take the broadest possible approach to malaria control. Brazil actually had to decentralize funding for malaria before it saw substantial reductions in malaria infections. PCMAM’s anti-malaria efforts included rapid diagnosis of malaria, preemptively treating all fevers with anti-malarial medications, controlling mosquitoes through spraying, eliminating the stagnant water they use to breed and strengthening malaria epidemiology and surveillance through collecting and reporting better data.
A vaccine for malaria is the holy grail of malaria control. Even a slightly effective vaccine could be the straw that breaks the back of malaria.
We may be seeing that happen. Right now, a malaria vaccine is being rolled out in Ghana, Kenya, and Malawi in a four-year pilot program that will run through 2022. This is the pilot introduction test of a vaccine called RTS,S. Thirty years in development, the vaccine is manufactured by GSK. It was developed by a partnership of organizations that included GSK, PATH’s Malaria Vaccine Initiative (with funding from the Gates Foundation), and a network of African research centers at 11 sites in 7 countries.
RTS,S is not going to transform malaria control. It is only 39% effective against malaria. It has been found to be less cost-effective in malaria prevention than bednets in most situations. But it is one more tool in a toolbox that has never had enough options. Sub-Saharan Africa bears most of the burden of malaria – the WHO African region contains 92% of all malarial infections and 93% of all deaths. These countries desperately need one more prevention approach.
RTS,S will be administered to children in a range of malarial transmission settings as part of routine vaccine programs. In its Phase Three clinical trial (phase three determines effectiveness after Phase Two makes sure it is safe), it was found that children who received four doses of the vaccine had a significantly reduced risk of developing malaria, including severe malaria.
RTS,S is not intended to take the place of other malarial control interventions. It is meant to be that last malaria-controlling straw.
In addition to helping to protect approximately one million babies from malaria over four years, the pilot program will establish the feasibility of adding a four-dose vaccine to the routine immunization schedule in poor countries, provide large scale data on the role the vaccine can play in reducing child deaths, and identify lessons learned from routine administration of the vaccine. The timeline for vaccine introduction will be randomized by district, to help collect the most detailed impact data possible. The World Health Organization (WHO) will use the data from this pilot program to issue a broad policy recommendation on the RTS,S vaccine and its use.
RTS,S will not be a silver bullet. It is only effective against the P. falciparum malaria infections common to Africa, not the P. vivax infections found in malarial hotspots in Southeast Asia. It also protects only 39% of children who are vaccinated from malaria. However, reducing malaria infections in four of every ten children is meaningful reduction in death and suffering in its own right. That reduction will also increase the impact of prevention efforts by reducing the number of infected individuals available for mosquitoes to bite and then spread the disease.
Fighting malaria has always been a game of small steps that accrue into real impact. RTS,S is a small step with the potential to push all the other steps further.